All procedure details are explained as done in our centre,
and as described in most of the literature consulted,
when otherwise,
we point out the difference.
Step 1: GETTING STARTED
The first step is to place a 6 French arterial introducer Super Arrow-Flex®,35 cmlong,
(Arrow®; PA,
USA) through the right common femoral artery and perform initial aortoiliac angiography using an injection of 18 mL of iodinated contrast Iomeron 300 (Bracco s.p.a.; Milan,
Italy) at a velocity of 18 mL/second under fluoroscopic guidance.
(Fig.
3 and 4)

Fig. 3: Initial materials used: 6 French arterial introducer Super Arrow-Flex® and iodinated contrast.

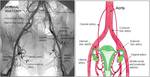
Fig. 4: Left: normal anatomy in an aortogram with internal iliac arteries and its anterior and posterior divisions.
Right: Schematic drawing of the anatomy.
Then a selective injection of contrast (12 mL at a velocity of 5 mL/sec.) into the left internal iliac artery is performed,
using a 4 or5FCobra© catheter (Terumo Europe;Leuven,Belgium) and its branches,
mainly the anterior division.
In some series,
the right internal iliac artery is catheterized first,
the order does not seem to affect the results of the procedure.
Step 2: VISUALIZE THE ANATOMY
In most cases,
the internal iliac artery terminates into 2 main stems,
an anterior (inferior) and a posterior (superior) division.
(Fig.
5) The uterine artery usually arises from the anterior division.
As a result,
its origin usually cannot be seen in anteroposterior views and an ipsilateral or contralateral anterior oblique projection should be used.
(Fig.
6)

Fig. 5: Drawing of the arterial anatomy of the female tract.
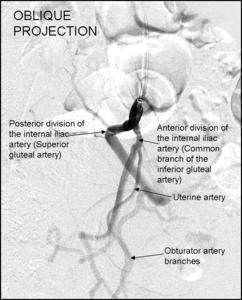
Fig. 6: The origin of the uterine artery from the anterior division of the iliac artery can be easily identified in the oblique projections.
The uterine artery is easy to identify due to its characteristic U-shaped course.
(Fig.
7)

Fig. 7: Left: Uterine artery with its characteristic U-shaped course. Right: Enlarged uterine artery in a puerperal patient since the uterus itself is increased.
Occasionally at this point active bleeding may be revealed which requires superselective catheterization (Fig.
8),
in which case a2,7FProgreat©130 cmlong catheter with a 0,21 guide (Terumo Europe;Leuven,Belgium) is used.
Although the most frequently affected vessel is the uterine artery,
selective embolization of other actively bleeding vessels can be performed,
such as the vaginal,
pudendal or vesical arteries.
(Fig.
9)

Fig. 8: Left: Superselective arteriography of right uterine artery.
Right: Contralateral uterine artery. No active extravasation of contrast was observed in this patient, both uterine arteries were embolized empirically.

Fig. 9: Left: Active extravasation of contrast and pseudoaneurysm of vesical artery. Right: Microcoil in pseudoaneurysm. In this case embolization Microcoils™ Soft Platinum Types were used (MWCE - 18S - 3,5 - 4 - C and MWCE - 18S - 3,0 - 7 - B) (Cook; Bjaeverkov, Denmark).
In most cases there is no active extravasation of contrast as the bleeding is often intermittent and the uterine arteries may undergo severe spasm,
so an empiric embolization of both uterine arteries should be carried out.
Step 3: EMBOLIZATION
Embolization is done with gelatin sponge or a Surgicel Nu-Knit® (Johnson &Johnson Medical;Switzerland) and should be of the anterior division of the internal iliac artery only,
preserving the posterior branches.
Gelatin sponge and other hemostatic products are used as the embolic material because of semipermanent occlusion of the vessels with a potential for recanalization between 1 to 6 weeks later (varies according to the literature),
preserving uterine vascularisation and future fertility.
That is why permanent embolic agents such as small embolic particles and coils should not be routinely used,
except when a pseudoaneurysm is identified which will require the permanent occlusion to prevent a recanalization of the lesion.
Preparation is made by cutting the Surgicel® with a pair of scissors,
in increasing sizes (1-1,5 mm) that are particularly suitable for leaving the capillary bed intact.
These are placed into an empty dish with approximately 10 mL of saline solution with 50% of contrast.
(Fig.
10 and 11)

Fig. 10: Steps in the preparation of the embolic material, in this case, Surgicel, cut in increasing sizes. Pour into an empty dish with saline solution and contrast.
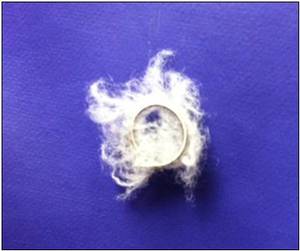
Fig. 11: Coil, permanent embolic material.
Step 4: REPEAT PROCEDURE
Contralateral internal iliac arteriography should be performed to repeat the procedure with the right uterine artery.
(Fig.
12)

Fig. 12: Left: Right internal iliac artery previous to embolization.
Right: Post-embolization.
Step 5: CHECK THE RESULTS
Aortography is repeated after the procedure to ensure that there is no residual extravasation of contrast agent.
Step 6: CLOSING UP
Remove the catheters and use a vascular closure device such as Angio-Seal™ VIP (St.
Jude Medical Europe;Zaventem,Belgium).
(Fig.
13) When using this type of device there is no need for manual compression,
unless there is bleeding at the closure site.

Fig. 13: Vascular closure device Angio-Seal™ VIP
If the procedure fails,
vascular ligations should then be considered and a second arterial embolization can be attempted.
Should these fail,
a hysterectomy can be performed.